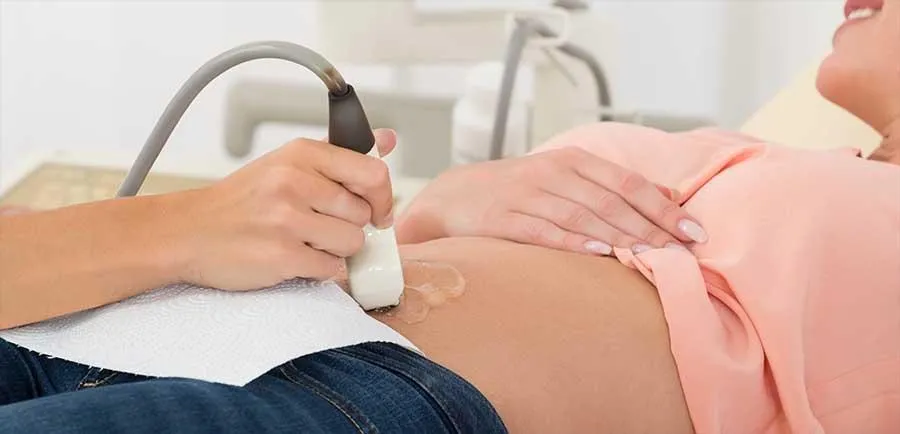
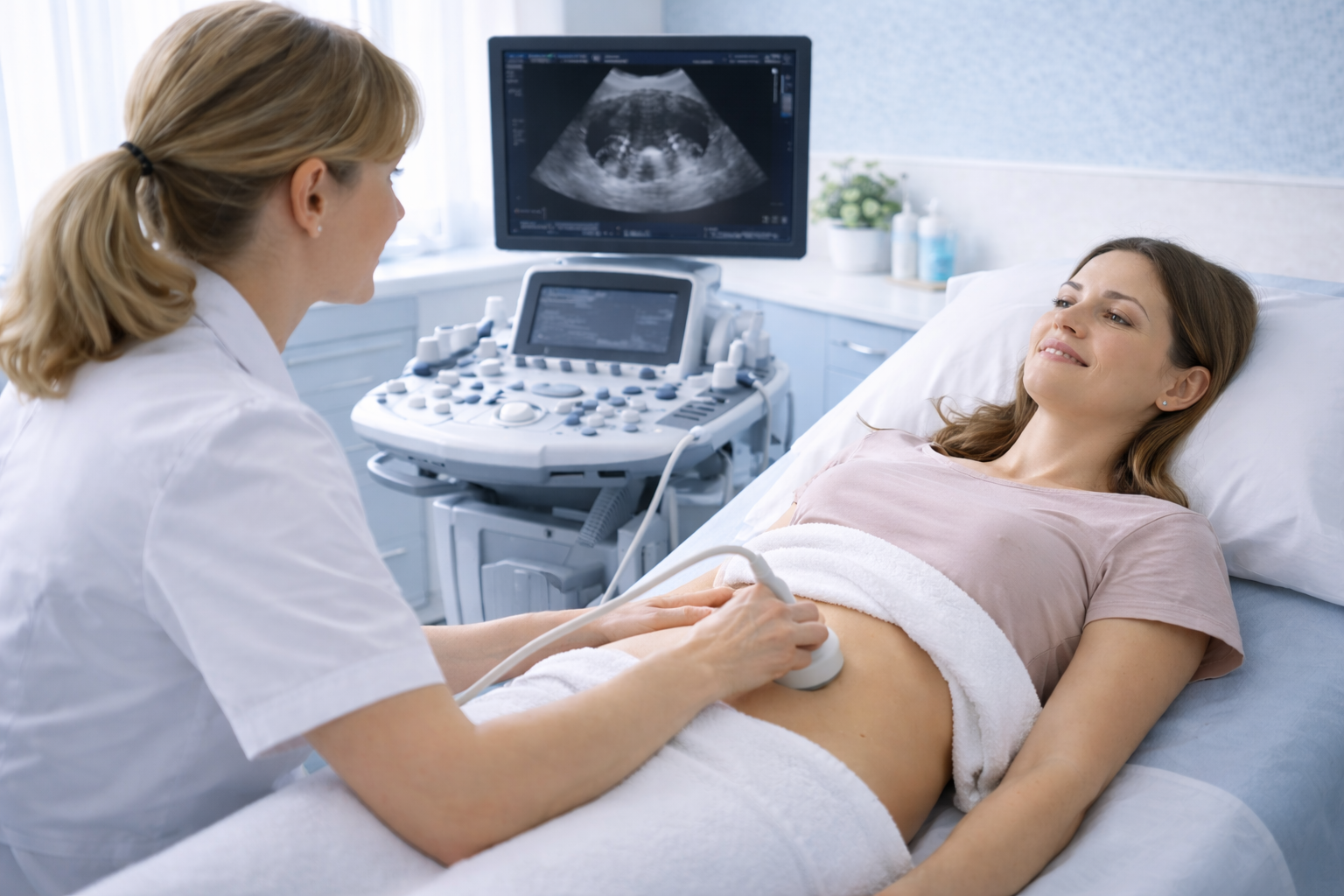
Uterus & endometrium
Size, shape and position of the uterus. The endometrial lining is measured: a key reading for heavy periods, irregular bleeding and postmenopausal bleeding. Fibroids, polyps and the MUSA-defined direct features of adenomyosis are identified and described.