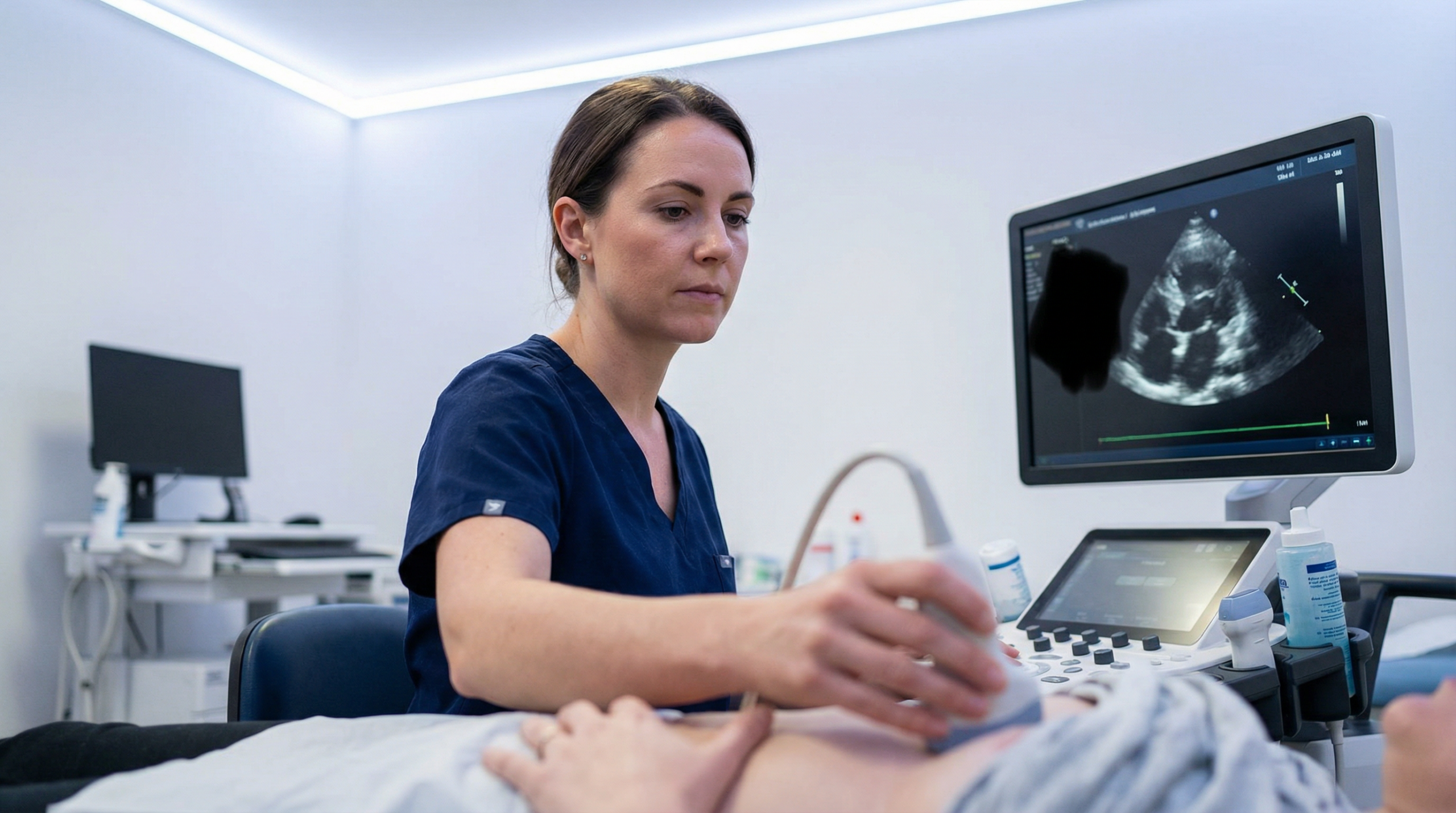
What are the main limitations of an echocardiogram?
An echocardiogram is a powerful and safe tool for looking at the heart. It can assess the size of the chambers, the function of the valves, the strength of the heart muscle, and the flow of blood — all in real time, without radiation, and at the bedside. For the majority of cardiac questions, it is the first-line imaging test recommended by the British Society of Echocardiography (BSE) and NICE.
Like any medical test, echocardiography has its limits. Understanding these helps you and your clinical team make informed decisions about your care. The limitations fall into three broad categories: factors related to the patient’s body, technical aspects of the ultrasound-scan itself, and specific clinical questions that echo is not designed to answer.

Ultrasound works by sending high-frequency sound waves into the body and listening to the echoes that bounce back from cardiac structures. For this to work well, there needs to be a clear path from the probe on the chest to the heart. This path is called the acoustic window. When the window is poor, the images can be blurry, incomplete, or difficult to interpret with confidence.
Several factors can reduce the quality of the acoustic window:
| Factor | How it affects the echo | Approximate prevalence |
|---|---|---|
| Obesity (BMI >30) | More tissue between the probe and the heart weakens the ultrasound signal and reduces image clarity. Studies show poor acoustic windows in up to 30% of obese patients. [1] | Common |
| COPD and emphysema | Hyperinflated lungs trap air between the ribs and the heart. Air blocks ultrasound waves almost completely, making it very difficult to get clear images from standard probe positions. | Common in moderate-to-severe COPD |
| Chest wall shape | Conditions like pectus excavatum (sunken chest) or kyphoscoliosis can alter the position of the heart relative to the chest wall, reducing the available acoustic windows. | Uncommon |
| Previous cardiac surgery | Scar tissue from a sternotomy or the presence of surgical material can interfere with sound wave transmission. | Common in post-surgical patients |
| Breast implants | Silicone or saline implants can block the ultrasound beam from certain angles, limiting the views available to the sonographer. | Uncommon |
| Mechanical ventilation | Positive-pressure ventilation can push the lungs over the heart, reducing the available windows. This is more relevant in intensive care settings. | Relevant in ICU patients |
Experienced sonographers are skilled at working around these challenges. Adjusting the patient’s position (lying on the left side is standard), using subcostal or suprasternal views, and applying harmonic imaging can all improve image quality. When the acoustic window is too poor for a diagnostic-quality study, contrast echocardiography — where a small amount of microbubble contrast agent is injected intravenously — can significantly enhance the images. If even that is insufficient, a different imaging modality such as cardiac MRI may be recommended.
Technical limitations of echocardiography
Even with a perfect acoustic window, there are inherent technical aspects of ultrasound that introduce limitations. These are well understood in clinical practice and are managed through standardised protocols, training, and quality assurance.
Operator dependence
Echocardiography is a highly operator-dependent investigation. The quality and accuracy of the study depend on the skill, training, and experience of the person performing it. Two sonographers scanning the same patient may obtain slightly different measurements — this is known as inter-observer variability. Even the same sonographer can produce slightly different results on a repeat study (intra-observer variability). For ejection fraction, the accepted inter-operator variability is approximately 5%. [2]
This is why accreditation matters. At Sonoworld, every echocardiogram is performed by Daniela Stan, a BSE-accredited consultant sonographer with over 20 years of clinical experience. Strict adherence to BSE protocols minimises variability and ensures consistent, reproducible results.
Measurement errors
Certain echocardiographic measurements are more susceptible to error than others. The diameter of the left ventricular outflow tract (LVOT), for example, is used to calculate cardiac output. Any error in this single measurement is squared in the final calculation — a 10% error in diameter produces approximately a 20% error in the calculated cardiac output. [2]
Doppler measurements require the ultrasound beam to be perfectly aligned with the direction of blood flow. A misalignment of just 30 degrees results in more than a 10% underestimation of blood flow velocity. Skilled sonographers use multiple views and angle-correction techniques to minimise this, but it remains an inherent limitation of the physics of Doppler ultrasound.
Geometric assumptions
The calculation of ejection fraction using the biplane Simpson’s method assumes a degree of symmetry in the shape of the left ventricle. In a healthy heart, this assumption holds well. After a heart attack, however, the ventricle may develop regional wall motion abnormalities or an aneurysm, distorting its shape. In these cases, the geometric model becomes less accurate, and the calculated EF may not fully represent the heart’s true pumping ability.
Three-dimensional (3D) echocardiography helps overcome this limitation by creating a volumetric model of the ventricle rather than relying on two cross-sectional planes. However, 3D echo requires a good acoustic window and uses a larger probe, which can itself be a limiting factor.
Not a continuous monitor
An echocardiogram provides a detailed snapshot of the heart at a specific moment in time. Unlike an ECG Holter monitor or continuous blood pressure recording, it cannot track changes over hours or days. For patients whose symptoms are intermittent — such as palpitations that come and go — the echo may appear entirely normal if the arrhythmia is not present during the study. Ambulatory monitoring is often needed alongside echocardiography to capture the full clinical picture.
When is another test better than an echocardiogram?
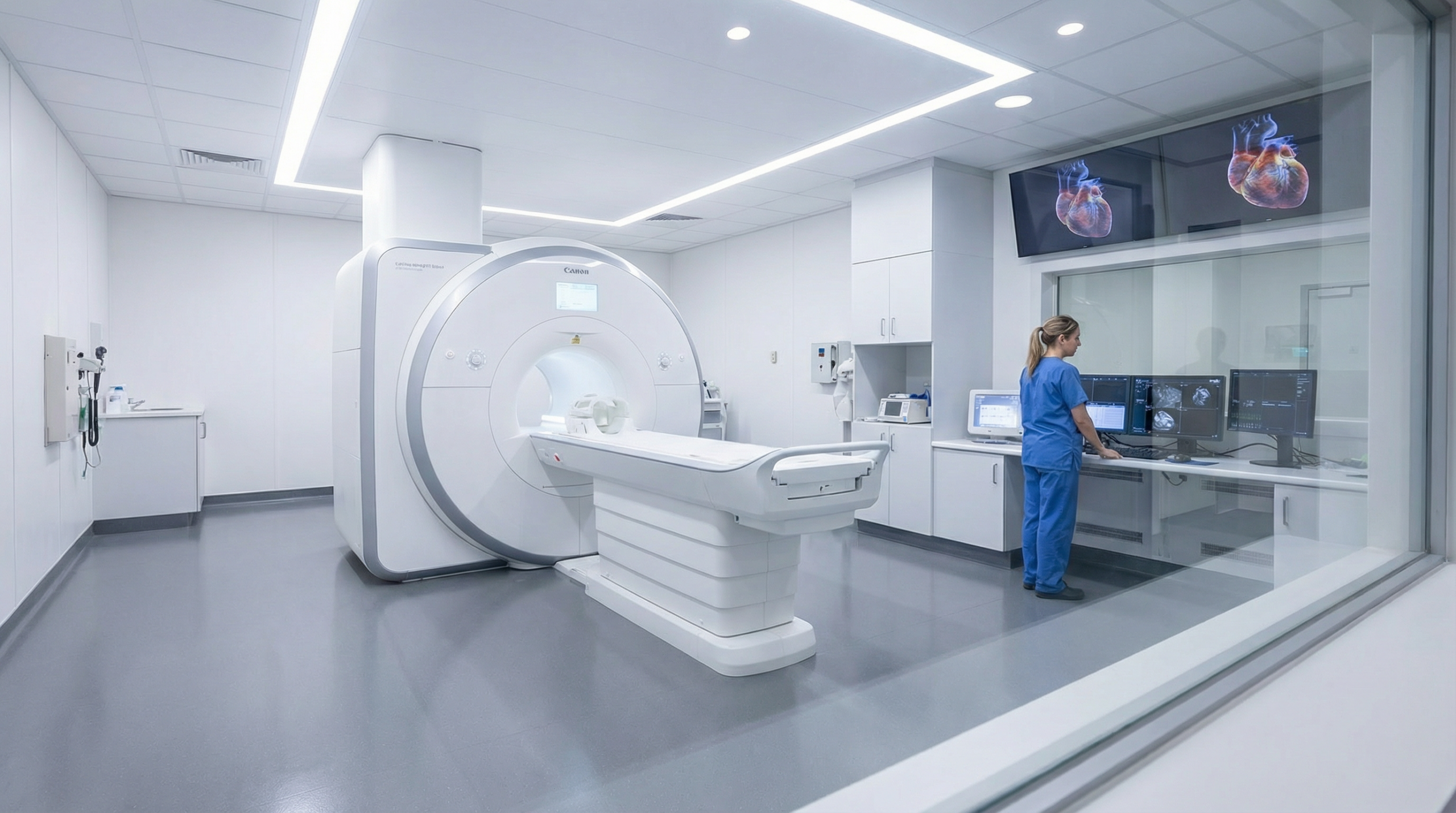
Echocardiography is the first-line imaging test for most heart conditions, but it cannot see everything. For certain clinical questions, other imaging modalities are the gold standard because they provide information that echo simply cannot deliver.
| Clinical question | Echocardiography (TTE) | Gold standard alternative |
|---|---|---|
| Are my coronary arteries blocked? | Cannot directly visualise the coronary arteries. Can only detect the effect of a blockage (e.g., a weak area of heart muscle). | Cardiac CT angiography (CTCA) — provides detailed 3D images of the coronary arteries to identify blockages directly. |
| Is there scar tissue in my heart muscle? | Cannot reliably distinguish between stunned (temporarily weakened but alive) muscle and dead scar tissue. | Cardiac MRI with contrast — late gadolinium enhancement directly shows areas of scar, which is important for prognosis and treatment planning. |
| What is the cause of my cardiomyopathy? | Can identify a thickened or enlarged heart muscle but often cannot determine the underlying cause (e.g., iron overload, amyloidosis, sarcoidosis). | Cardiac MRI — superior for tissue characterisation, helping to diagnose specific types of cardiomyopathy without needing a biopsy. |
| How is my right ventricle functioning? | The right ventricle has a complex, crescent shape that is difficult to assess fully with 2D echo. | Cardiac MRI — considered the gold standard for measuring the size and function of the right ventricle. |
| Do I have constrictive pericarditis? | Can show signs suggestive of constriction but cannot accurately measure the thickness of the pericardium (the sac around the heart). | Cardiac CT or MRI — directly measures pericardial thickness and shows other classic signs of constriction. |
| Is there a problem with my aorta beyond the root? | Provides excellent views of the aortic root but cannot see the entire aortic arch or descending thoracic aorta. | Cardiac CT or transoesophageal echo (TOE) — provides a complete view of the entire thoracic aorta. |
| Do I have endocarditis (valve infection)? | TTE can miss small vegetations (less than 2–3mm) on heart valves. Sensitivity is approximately 50–60%. | Transoesophageal echo (TOE) — the probe is passed down the oesophagus, providing much higher resolution images. Sensitivity exceeds 90%. |
Echocardiogram vs cardiac MRI: a detailed comparison
Cardiac MRI (CMR) and echocardiography are complementary, not competing, tests. Each has strengths the other lacks. The table below summarises the key differences to help you understand why your clinician may recommend one over the other — or both.
| Feature | Echocardiogram (TTE) | Cardiac MRI (CMR) |
|---|---|---|
| How it works | Sound waves (ultrasound) | Magnetic field and radio waves |
| Radiation | None | None |
| Real-time imaging | Yes — live images of blood flow and valve movement | No — images are reconstructed from multiple cardiac cycles |
| Tissue characterisation | Limited | Excellent — can detect scar, fibrosis, oedema, iron overload |
| EF accuracy | Good (biplane Simpson’s method) | Gold standard (volumetric measurement) |
| Right ventricle assessment | Limited by complex RV geometry | Gold standard |
| Valve assessment | Excellent — real-time Doppler flow | Good, but less practical for real-time haemodynamics |
| Portability | Portable — can be done at the bedside | Fixed installation — requires a dedicated MRI suite |
| Duration | 30–45 minutes | 45–90 minutes |
| Contraindications | None | Certain pacemakers, metallic implants, severe claustrophobia |
| Cost | Lower | Significantly higher |
| Availability | Widely available — including private clinics like Sonoworld | Limited to hospitals and specialist imaging centres |
Echocardiogram vs cardiac CT
Cardiac CT is a fundamentally different type of imaging that uses X-rays to create cross-sectional images of the heart and blood vessels. Its primary strength lies in visualising the coronary arteries — something echocardiography cannot do. Cardiac CT angiography (CTCA) is the non-invasive test of choice for ruling out coronary artery disease in patients with chest pain.
Cardiac CT also excels at measuring pericardial thickness, assessing the thoracic aorta, quantifying coronary artery calcium (calcium scoring), and planning for procedures like transcatheter aortic valve implantation (TAVI). The trade-off is that cardiac CT involves ionising radiation and often requires an iodine-based contrast agent, which may not be suitable for patients with kidney problems or contrast allergies.
For assessing heart function, valve disease, and blood flow, echocardiography remains superior. The two tests answer different questions and are often used together in a multimodality imaging approach.
Transthoracic echo (TTE) vs transoesophageal echo (TOE)
A standard echocardiogram is performed from the outside of the chest (transthoracic, or TTE). A transoesophageal echocardiogram (TOE) involves passing a small ultrasound probe down the oesophagus — the food pipe that sits directly behind the heart. This gives the probe a much closer view of certain structures, particularly the mitral valve, the left atrial appendage, the interatrial septum, and prosthetic heart valves.
TOE is not a replacement for TTE. It is a more invasive procedure that requires sedation and carries a small risk of oesophageal injury. TOE is recommended in specific clinical scenarios:
- Suspected endocarditis: TOE detects vegetations with a sensitivity exceeding 90%, compared with approximately 50–60% for TTE.
- Prosthetic valve assessment: Mechanical valve components create acoustic shadows that obscure TTE images. TOE provides a clear view from behind the valve.
- Pre-operative mitral valve assessment: Detailed views of the mitral valve anatomy are needed before surgical repair.
- Stroke workup: TOE is the best test for detecting a patent foramen ovale (PFO) or left atrial appendage thrombus as potential sources of embolism.
- Intraoperative guidance: TOE is used during cardiac surgery and catheter-based interventions to guide the procedure in real time.
Sonoworld performs transthoracic echocardiograms. If your clinical situation requires a TOE, we will clearly explain why and help facilitate a referral to an appropriate centre.
The Sonoworld approach: a commitment to clinical accuracy

At Sonoworld, we believe in using the right tool for the right question. Echocardiography is our primary diagnostic tool, and our clinical team, led by Daniela Stan, understands both its strengths and its limitations.
Our commitment to you includes:
- Expertise: Recognising when a poor acoustic window or a specific clinical question means that an echocardiogram alone is not sufficient for a confident diagnosis.
- Honesty: Clearly explaining the limitations of the test in your report and discussing why a different imaging modality might be better suited to answer your clinical question.
- Collaboration: Working with your GP or cardiologist to facilitate a referral for more advanced imaging like cardiac MRI or CT when it is clinically indicated.
An echocardiogram provides a wealth of information about your heart. Knowing what it can’t tell you is just as important as knowing what it can. This awareness ensures a more accurate diagnosis and a better care pathway for you.
Book your echocardiogram
No GP referral required. Same-day and next-day appointments available at our Marylebone clinic. Self-pay and insured patients accepted.
Frequently asked questions
If I have COPD, does that mean I cannot have an echocardiogram?
Is a transoesophageal echo (TOE) better than a normal echocardiogram?
Why can an echocardiogram not see my coronary arteries?
If my echocardiogram is normal, does that mean my heart is completely healthy?
What is the difference between an echocardiogram and a cardiac MRI?
Can I have a cardiac MRI at Sonoworld?
References
- Mavrogeni, S. I., et al. (2021). “Cardiovascular Imaging in Obesity.” Journal of Clinical Medicine, 10(6), 1249. PMC7996902
- Huang, S. J., & McLean, A. S. (2012). “Appreciating the Strengths and Weaknesses of Transthoracic Echocardiography in Hemodynamic Assessments.” Cardiology Research and Practice, 2012, 894308. Wiley Online Library