- Home
- Women
- Men
- MSK
- Cardiovascular
- Screening
- About
- Book a Scan
- Blog
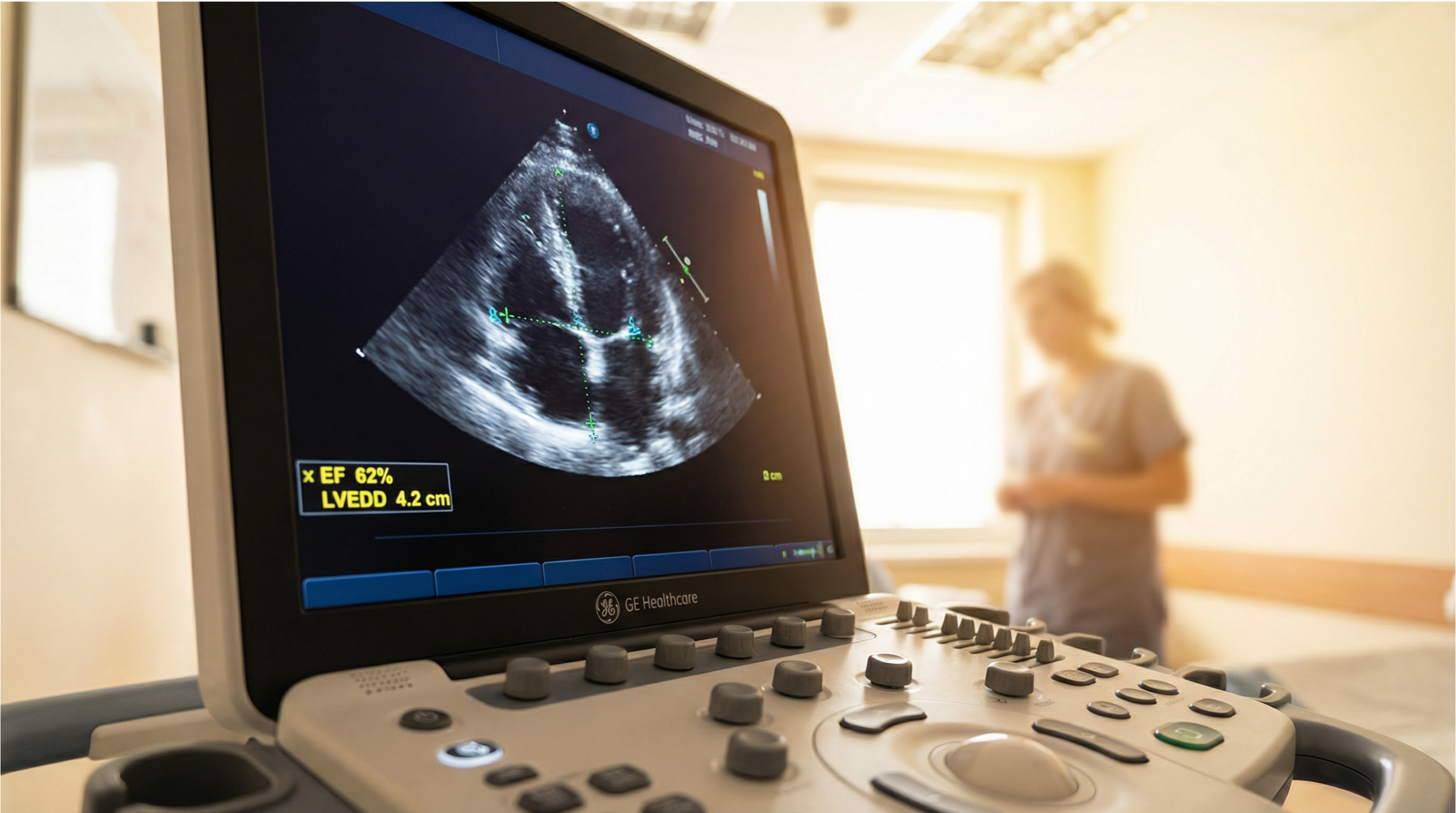
Left ventricular ejection fraction (LVEF) is the most important measurement used to diagnose and classify heart failure. This guide explains what your ejection fraction percentage means, how it is measured using an echocardiogram, and how it determines your treatment options.
Receiving a heart failure diagnosis or being told your heart is not pumping effectively can be an overwhelming and frightening experience. The terminology used by cardiologists can often feel confusing, leaving patients anxious about what their numbers actually mean for their daily life and future.
At Sonoworld Diagnostic Services in London, our consultant sonographers bring over 15 years of NHS and private clinical experience to every assessment. We provide rapid, same-day echocardiogram appointments without the need for a GP referral, ensuring you receive accurate diagnostic answers and a clear explanation of your results immediately. Our care is strictly aligned with the latest NICE and European Society of Cardiology guidelines.
Secure online booking. Results available within 24 hours.
Ejection fraction (EF) is a measurement, expressed as a percentage, of how much blood the left ventricle pumps out with each contraction. The left ventricle is the heart's main pumping chamber, responsible for supplying oxygen-rich blood to the rest of the body.
A normal heart does not pump out 100% of the blood it holds. A healthy ejection fraction is typically between 50% and 70%. This means that with each heartbeat, the left ventricle pumps out 50% to 70% of the blood it contains. When the ejection fraction drops below 50%, it indicates that the heart muscle has become weakened or damaged, a condition known clinically as systolic dysfunction (impaired pumping ability) [1].
Left ventricular ejection fraction (LVEF) is the primary parameter used by cardiologists worldwide to diagnose heart failure, determine the specific subtype of the disease, and guide treatment decisions. It is the most critical number on your echocardiogram report [2].

The Universal Definition of Heart Failure classifies the condition into distinct categories based entirely on your ejection fraction percentage. This classification is crucial because the medications and treatments prescribed differ significantly between the groups [3].
| Classification | Ejection Fraction (LVEF) | What it Means | Primary Treatment Focus |
|---|---|---|---|
| HFrEF (Reduced EF) |
40% or less | The heart muscle is significantly weakened and cannot contract forcefully enough to pump sufficient blood. Often caused by a previous heart attack or dilated cardiomyopathy. | Guideline-directed medical therapy (GDMT) including Beta-blockers, ARNIs, MRAs, and SGLT2 inhibitors to improve survival and heart function [1]. |
| HFmrEF (Mildly Reduced EF) |
41% to 49% | A transitional or "grey zone" where the heart's pumping ability is mildly impaired. Patients in this category often share clinical characteristics with HFrEF patients [4]. | Similar medications to HFrEF, focusing on preventing further decline in heart function and managing underlying conditions like coronary artery disease. |
| HFpEF (Preserved EF) |
50% or higher | The heart pumps normally, but the muscle has become stiff and cannot relax properly to fill with enough blood between beats (diastolic dysfunction). | Managing symptoms with diuretics, controlling blood pressure, and using SGLT2 inhibitors, which have recently shown significant benefit for this group [2]. |
| HFimpEF (Improved EF) |
>40% (previously ≤40%) | A new classification for patients whose ejection fraction was previously reduced but has improved by at least 10 points due to successful medical treatment [3]. | Continuing the current medical therapy to maintain the improvement and prevent relapse. |
Whether your ejection fraction is reduced (HFrEF) or preserved (HFpEF), the resulting heart failure syndrome produces similar symptoms because the body is not receiving the oxygen-rich blood it requires.
Feeling short of breath during everyday activities, such as walking up stairs or carrying groceries. In more advanced stages, breathlessness may occur while resting or lying flat in bed (orthopnoea).
Read about cardiac breathlessnessWhen the heart pumps less effectively, fluid backs up in the veins, causing swelling in the ankles, lower legs, and abdomen. You may also notice sudden, unexplained weight gain.
Read about leg swelling causesA persistent, overwhelming sense of tiredness and weakness that does not improve with rest. This occurs because the body diverts blood away from less vital organs (like muscles) to supply the brain and heart.
A sensation that your heart is racing, fluttering, or skipping beats. A reduced ejection fraction increases the risk of developing arrhythmias, such as atrial fibrillation.
Read about heart palpitationsAn echocardiogram (ultrasound-scan of the heart) is the gold standard, non-invasive test used to measure your left ventricular ejection fraction and diagnose heart failure. It is painless, involves no radiation, and provides immediate results.
At Sonoworld, your assessment begins with a detailed clinical history. Our consultant sonographer will ask about your symptoms, exercise tolerance, and family history. During the ultrasound-scan, you will lie on your left side while a small probe (transducer) is moved across your chest.

A heart failure diagnosis requires a comprehensive, individualised approach. At Sonoworld, we believe in empowering patients with clear information so they can actively participate in their care plan.
Treatment is not just about improving the ejection fraction number; it is about improving your quality of life. Care plans are built around measurable targets, such as:
We provide a multidisciplinary approach to diagnostics. Our consultant sonographers work closely with referring GPs and consultant cardiologists to ensure seamless continuity of care. We adhere strictly to clinical governance standards, ensuring that your diagnostic report is comprehensive, accurate, and immediately available to guide your prescribing clinician.