- Home
- Women
- Men
- MSK
- Cardiovascular
- Screening
- About
- Book a Scan
- Blog
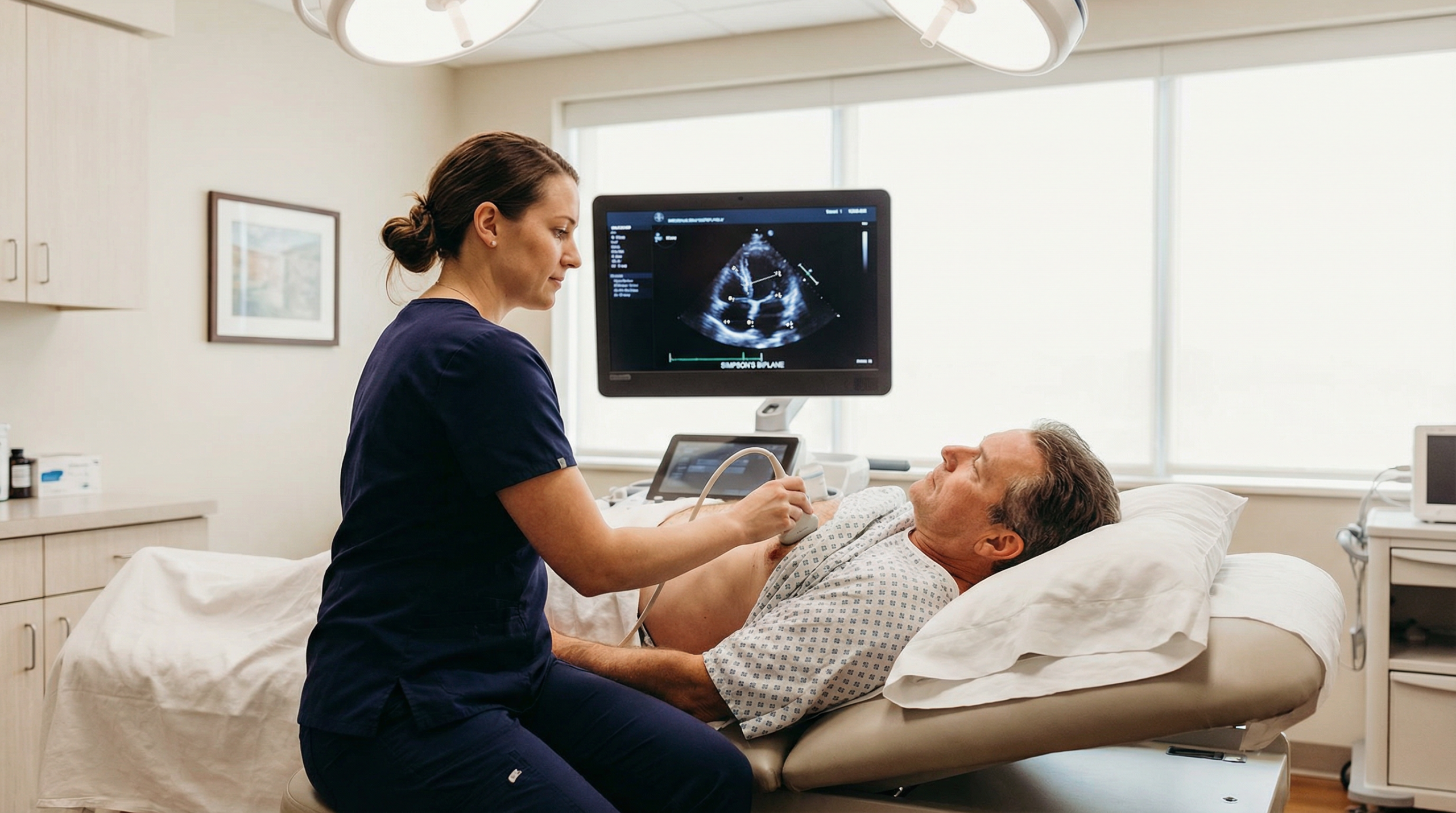
If you’re dealing with breathlessness, palpitations, dizziness, a new murmur, or you just feel “something isn’t right” — you want a test that answers the right question. This guide shows which symptoms echocardiography is designed to investigate, what it can and can’t clarify, and the safest next step if your symptoms are urgent.
If you have severe chest pain, severe breathlessness at rest, collapse, or you feel acutely unwell, seek urgent medical care first. A private scan is for clarity and next-step guidance — not emergency treatment.
This page is here to reduce uncertainty — not to push you into the wrong pathway. If any of the situations below fit, treat it as a safety-first moment and seek urgent medical care.
A transthoracic echo (TTE) is excellent for structure and function. But if your symptoms suggest an acute event, the priority is immediate clinical assessment and the right time-critical tests.
Echo safety and risks (plain English) Limitations of echocardiography (what it can’t show)Think of an echo as a “moving heart assessment”. If the question is about pumping, valves, heart size or fluid around the heart, an echo is often a strong first imaging step.
| Symptom / trigger | Typical pathway | Why echo helps | Practical next step |
|---|---|---|---|
| New or worsening breathlessness (especially on exertion) | Book soon | Assesses pumping function, valve disease, chamber size, and pericardial fluid. | Echo + clinical review. If breathlessness is severe at rest or rapidly worsening: urgent care first. |
| Palpitations with dizziness or reduced exercise tolerance | Book soon | Checks structural contributors (valves, cardiomyopathy patterns) and baseline function. | Often best combined with ECG/rhythm monitoring. Echo vs ECG. |
| Heart murmur found on examination | Book soon | Directly evaluates valve opening/closing, narrowing, and leakage with Doppler. | Echo is commonly the next step. See conditions diagnosed by echo. |
| Swollen ankles/legs with a cardiac query | Depends | Can support heart-failure assessment when combined with symptoms and history. | If swelling is one-sided with pain/redness: you may need a clot pathway. Consider vascular assessment. |
| Chest symptoms (non-acute) or reduced exercise capacity | Depends | Echo can show consequences (function, valves), but doesn’t directly image coronary arteries. | If coronary disease is the main concern, CT/other pathways may be used. Echo vs CT. |
| Known heart condition needing monitoring (as advised) | Book soon | Tracks function, chamber size, valve severity trends, and response to treatment. | Echo at the interval recommended by your clinician. Keep copies of prior reports for comparison. |
| Severe chest pain, collapse, severe breathlessness at rest | Urgent care | Echo may be used in hospital assessment — but the priority is emergency evaluation. | Seek urgent medical care immediately. |
Breathlessness is one of the most common reasons people book an echo — and one of the easiest symptoms to misinterpret. Echo is useful when the question is: “Could this be related to heart function or valves?”
Echo doesn’t diagnose every cause of breathlessness. It answers the heart-specific part of the question: how well your heart pumps, how the valves behave, and whether there’s fluid around the heart.
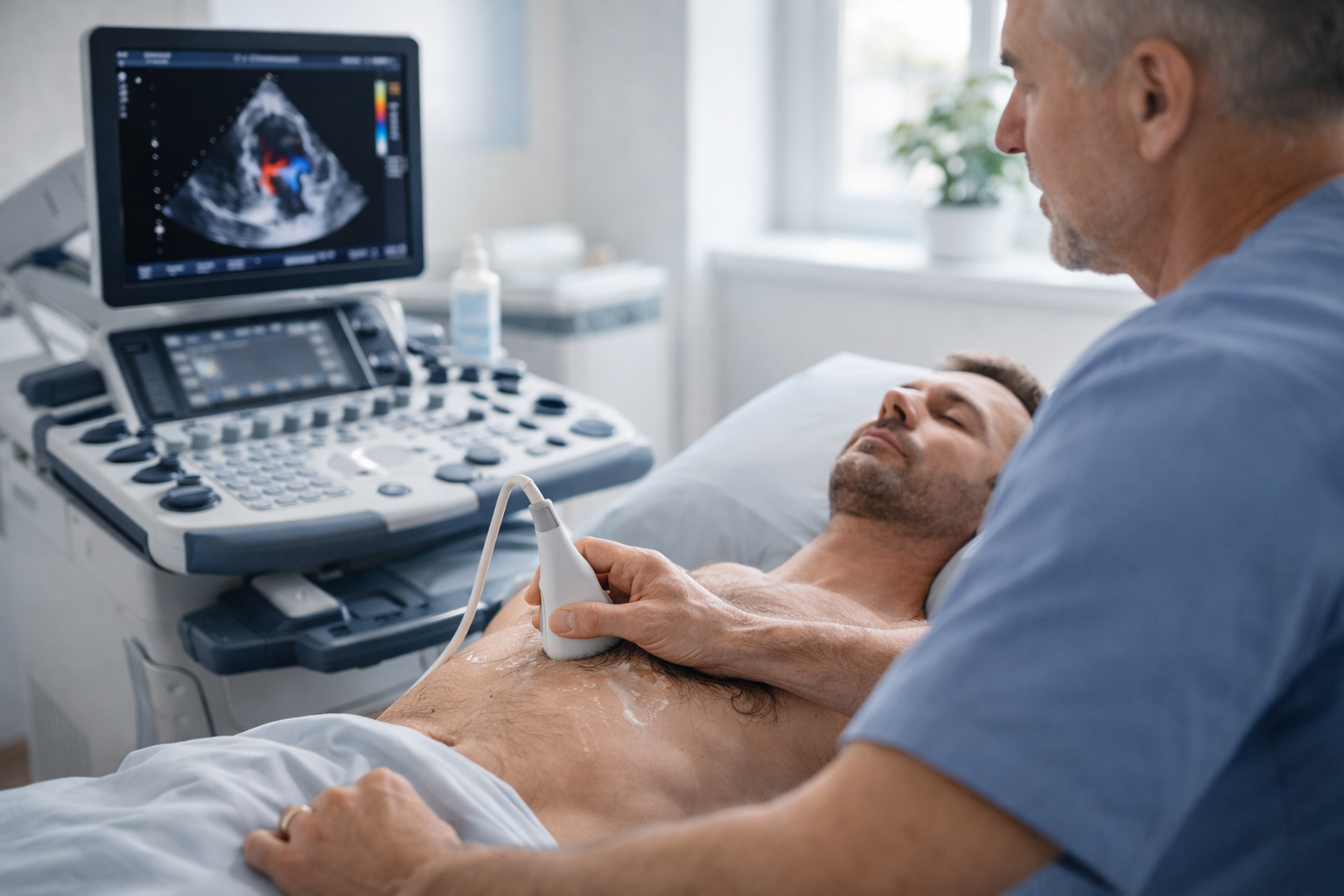
Palpitations are usually an electrical rhythm question first — that’s where ECG and rhythm monitoring shine. Echo becomes important when we need to check whether there’s a structural reason the rhythm is misbehaving.
People book an echo expecting it to “catch” a rhythm problem. Echo is a snapshot of structure and function. Rhythm capture is an ECG/monitoring job. If the symptom is episodic palpitations, consider pairing the pathways.
What an ultrasound echo actually measuresA murmur is a sound — echo is how we figure out what’s behind it. In practical terms, echo checks whether a valve is narrowing, leaking, or simply creating harmless flow noise.
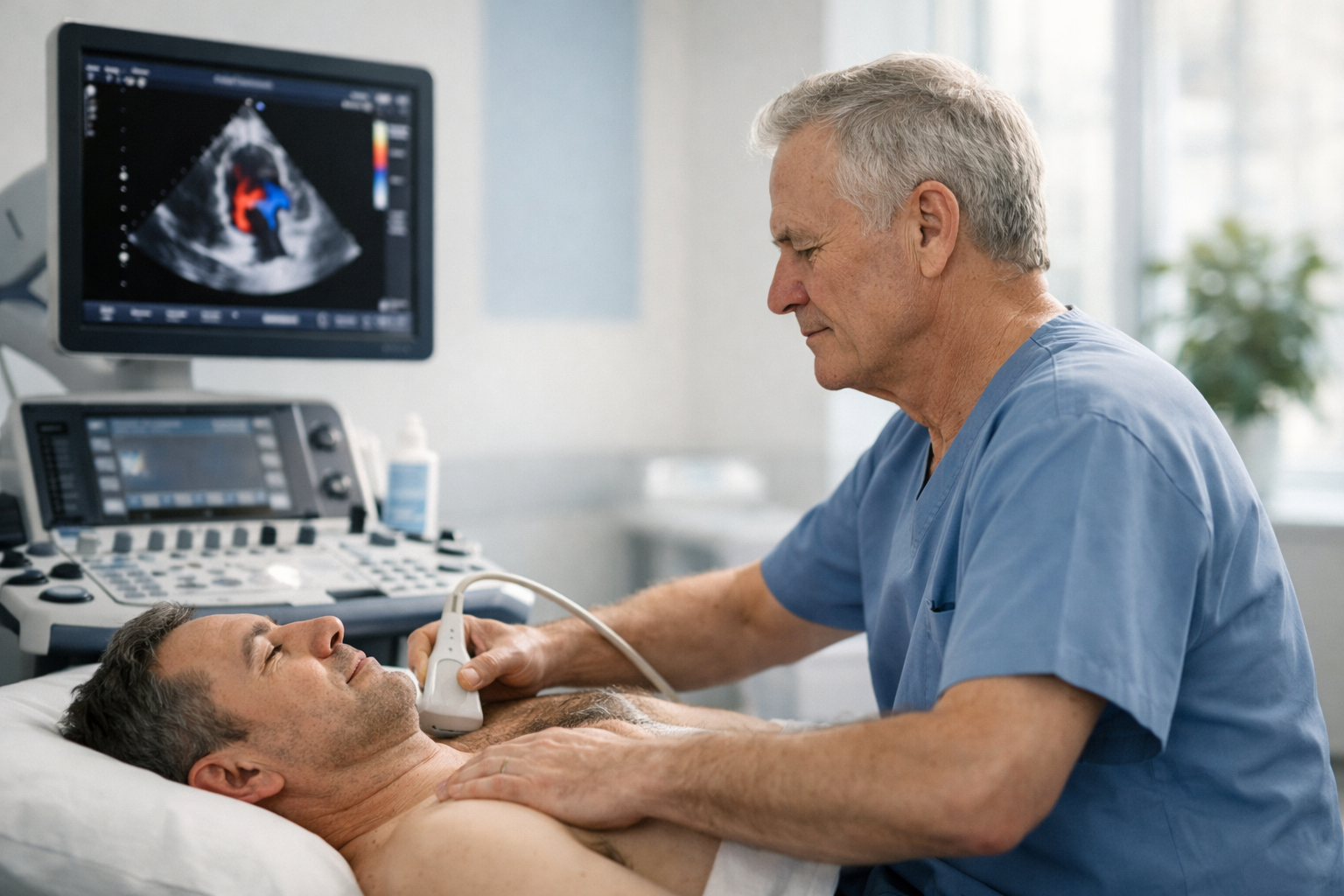
Swelling can be cardiac, vascular, kidney-related, medication-related, or due to prolonged sitting/standing. Echo contributes when the clinical question is heart function and valve status — but it’s not the best test for every swelling scenario.
One-sided swelling with pain, redness, or warmth can be a clot pathway. That usually needs urgent clinical assessment and/or a DVT ultrasound route. If you’re unsure, call and describe your symptoms so you’re directed correctly.
Explore vascular scans (circulation-focused)
People often book an echo hoping it will rule out “blockages”. Echo is a function/structure test. If your main worry is coronary artery disease, clinicians may use ECG, blood tests, CT coronary angiography or stress pathways depending on your symptom pattern and risk profile.
If the question is “is my heart pumping normally?” or “is a valve the issue?”, echo is a strong option. If the question is “are my coronary arteries narrowed?”, echo is not the direct test.
Echo vs CT: anatomy vs function (and why it matters)This is the moment most people want: a simple, respectful process with a clear output. Here’s what the appointment typically looks like, and how the report is used.
If you’re using insurance, check whether you need authorisation before booking. Prefer to talk it through first? Call 020 3633 4902.
An echo rarely “stands alone”. It sits inside a pathway: symptoms → the right test → the right next step. If your symptom is mainly electrical (palpitations), you’ll often need ECG/rhythm capture. If it’s mainly coronary concern, CT/stress pathways may be needed.
Echo vs ECG Limitations of echocardiographyShort answers, no fluff.