- Home
- Women
- Men
- MSK
- Cardiovascular
- Screening
- About
- Book a Scan
- Blog
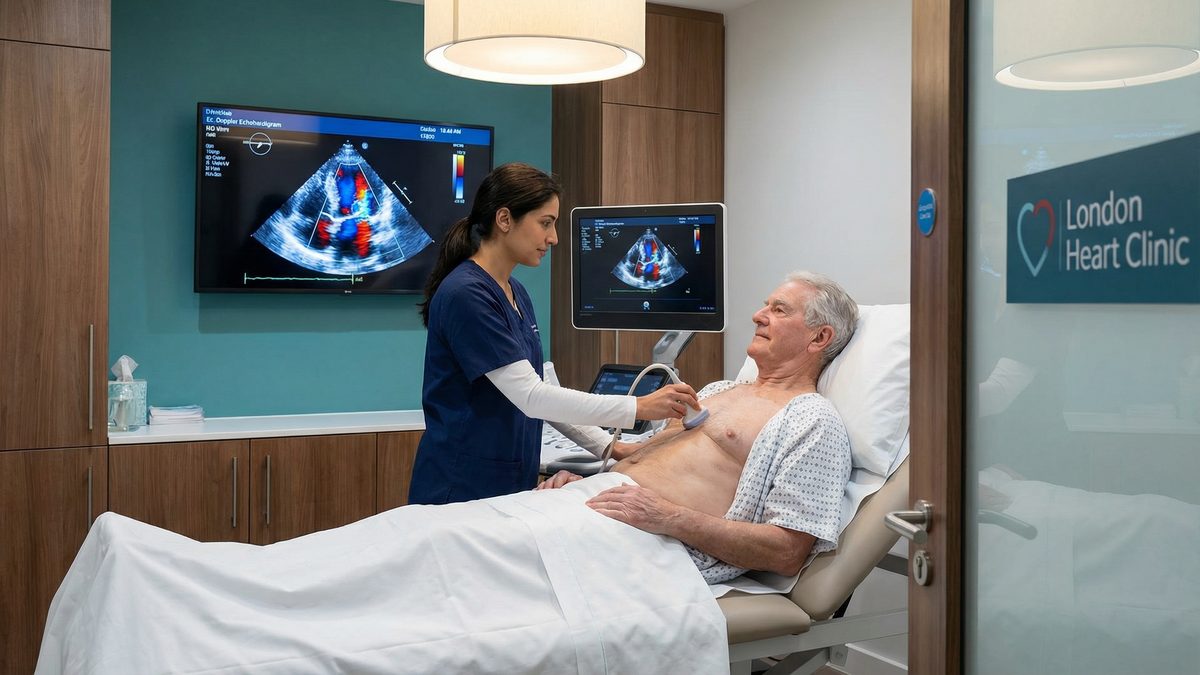
Aortic stenosis is the most common valvular heart disease in the UK, affecting a significant proportion of the older population. It occurs when the heart's aortic valve narrows, restricting blood flow from the heart to the rest of the body. This comprehensive guide explains the causes, symptoms, and how an echocardiogram is used to accurately grade the severity of the condition.
The aortic valve is the final gateway between the heart and the rest of the body. When the heart's left ventricle contracts, the aortic valve opens to allow oxygen-rich blood to flow into the aorta (the main artery). Aortic stenosis occurs when the leaflets of this valve become stiff, thick, or fused together, narrowing the opening.
This narrowing forces the heart muscle to work significantly harder to pump blood through the restricted valve. Over time, this increased workload causes the heart muscle to thicken (left ventricular hypertrophy) and eventually weaken, leading to heart failure if left untreated. A large-scale study of nearly 30,000 echocardiograms found that 7.2% of patients had some degree of aortic stenosis, with the prevalence rising sharply in those over 75 years of age [1].
Aortic stenosis is often described as a "silent" disease because it progresses slowly over many years. The heart compensates for the narrowing valve by thickening its muscle walls. During this compensatory phase, patients may feel completely normal and remain asymptomatic.
However, once symptoms do appear, the condition has typically reached a severe stage, and the prognosis without intervention declines rapidly. This highlights the importance of early detection through an echocardiogram, especially if a doctor detects a heart murmur during a routine stethoscope examination.

The onset of symptoms in aortic stenosis is a critical clinical milestone. Research shows that the severity of presenting symptoms directly correlates with long-term survival outcomes, even after the valve is replaced [2].
If you experience sudden, severe chest pain, fainting (syncope), or extreme difficulty breathing, call 999 immediately. These can be signs of critical aortic stenosis or a heart attack.
Initially noticed only during physical exertion, such as climbing stairs. As the condition worsens, shortness of breath may occur at rest or when lying down. This is often a sign that fluid is backing up into the lungs (heart failure).
A feeling of tightness, pressure, or squeezing in the chest, particularly during activity. This occurs because the thickened heart muscle requires more oxygen than the narrowed coronary arteries can supply.
Feeling dizzy, lightheaded, or completely losing consciousness, especially during or immediately after physical exertion. This happens when the narrowed valve prevents the heart from pumping enough blood to the brain.
A profound sense of tiredness and a noticeable decline in the ability to perform normal daily activities. Patients often subconsciously reduce their activity levels to avoid triggering other symptoms.
An echocardiogram is the primary and most important diagnostic tool for aortic stenosis. This specialised ultrasound-scan allows cardiologists to directly visualise the valve, measure the severity of the narrowing, and assess how well the heart muscle is coping with the increased workload.
During the scan, the sonographer will use Doppler ultrasound to measure three critical parameters that determine the severity of the stenosis:
Grading aortic stenosis is not always straightforward. In approximately 25% of patients with severe stenosis, the pressure gradient appears deceptively low (under 40 mmHg) despite a critically narrowed valve area (under 1.0 cm²) [1].
This condition, known as Low-Flow, Low-Gradient (LFLG) severe aortic stenosis, occurs when the heart muscle has become too weak to generate a high pressure gradient. These patients represent a diagnostic challenge and often require advanced echocardiographic techniques or a cardiac CT scan to confirm the severity of the calcification and ensure they receive timely treatment [4].

There are no medications that can reverse or slow the progression of aortic valve narrowing. Once severe aortic stenosis becomes symptomatic, the only effective treatment is to replace the diseased valve. Without valve replacement, the prognosis is poor, with a high mortality rate within two to three years of symptom onset.
| Procedure | How it works | Recovery Time | Best suited for |
|---|---|---|---|
| TAVI (Transcatheter Aortic Valve Implantation) |
A minimally invasive procedure. A new valve is delivered via a catheter, usually inserted through an artery in the groin, and expanded inside the old, diseased valve. | Typically 2 to 5 days in hospital. Faster return to normal activities. | Patients of all surgical risk levels. Recent landmark trials have proven TAVI is non-inferior to open surgery even in low-risk patients [5] [6]. |
| SAVR (Surgical Aortic Valve Replacement) |
Traditional open-heart surgery. The chest is opened, the patient is placed on a bypass machine, the diseased valve is removed, and a new mechanical or tissue valve is sewn in. | Typically 7 to 10 days in hospital. Several weeks for full sternum healing. | Younger patients, those needing a mechanical valve, or patients requiring other simultaneous heart surgeries (e.g., coronary bypass). |