
Repeat ECG (12-lead)
Useful if the first recording had artefact, symptoms have changed, or a clinician wants to compare patterns.
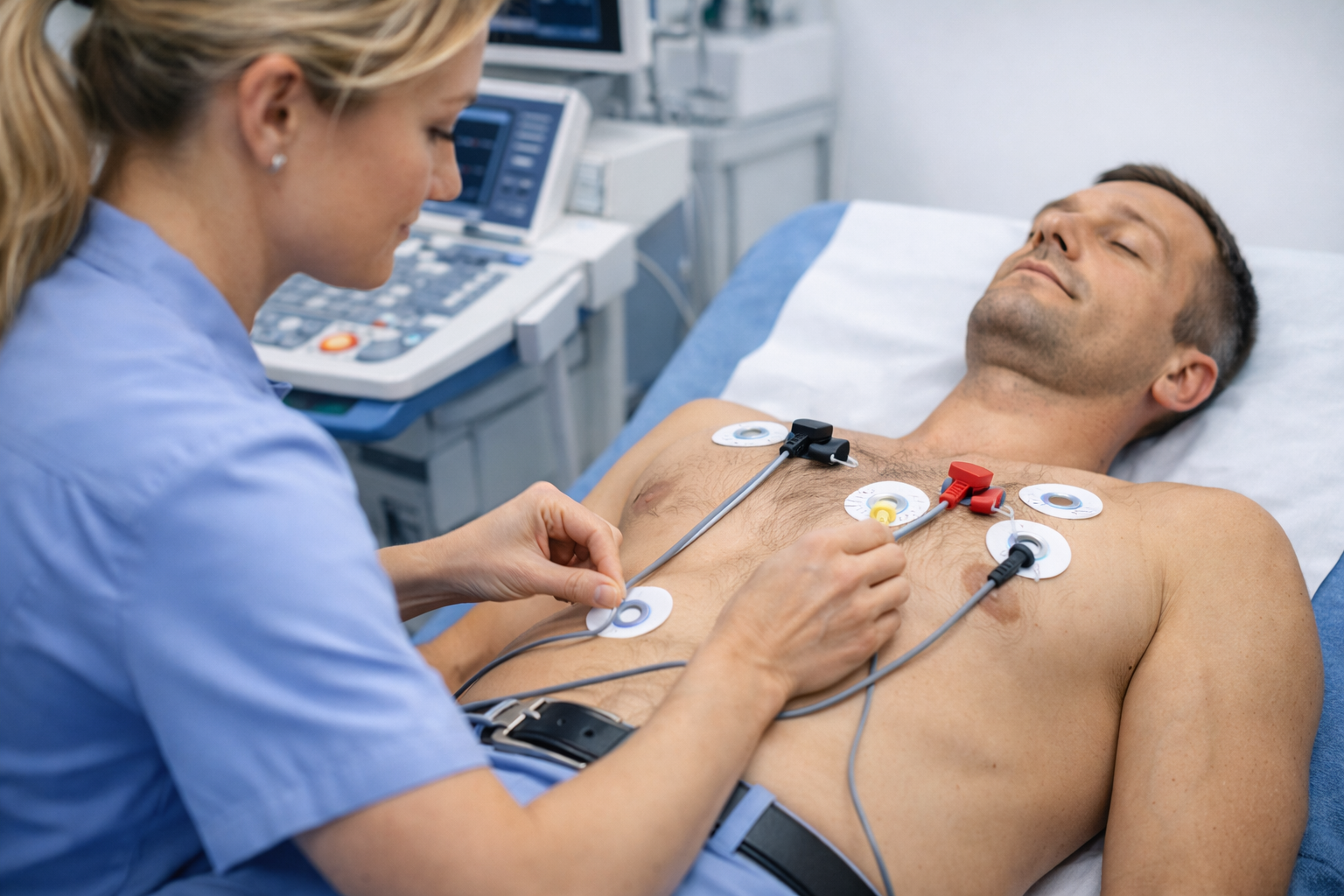
Seeing the word “abnormal” on an ECG report can be unsettling — but it doesn’t automatically mean you have heart disease. This guide explains the most common reasons an ECG is flagged, what your result might be pointing towards, and what to do next (including when you should seek urgent help).
If you also have chest pain, severe breathlessness, fainting, or new weakness on one side, don’t wait for a guide — call 999 or go to A&E.
An ECG (electrocardiogram) is a snapshot of your heart’s electrical activity at one moment in time. Software (and sometimes clinicians) use the word abnormal when the pattern falls outside a standard range — but that range doesn’t perfectly fit every person.
If you feel well and the ECG was done as a routine check, an “abnormal” label usually means: “Let’s confirm what this is” rather than “Something is definitely wrong.”
If symptoms brought you to the ECG (palpitations, chest pain, breathlessness, fainting), the same “abnormal” word carries more weight — because symptoms change the risk picture.
Below are the patterns that most often trigger an “abnormal” report. The key word is can — the same finding can be harmless in one person and significant in another.
| ECG wording you might see | What it often points to | What usually happens next |
|---|---|---|
| Sinus bradycardia Slow rhythm from the normal pacemaker |
Common in fit people; can also relate to medications or conduction changes. | Review symptoms (dizziness/fainting). Consider Holter if symptoms come and go. |
| Sinus tachycardia Fast rhythm from the normal pacemaker |
Stress, pain, fever, dehydration, anaemia, thyroid overactivity — not always a heart problem. | Check triggers, basic observations, and sometimes blood tests. Repeat ECG if needed. |
| Premature beats (ectopics) PACs/PVCs |
Extra beats; often benign. More important if frequent, symptomatic, or with dizziness/fainting. | Holter monitoring is usually the best next test to measure “how many” and link to symptoms. |
| Atrial fibrillation / flutter | Irregular rhythm; may increase stroke risk and cause breathlessness or fatigue. | Clinical review. Often needs medication discussion and sometimes an echo to assess structure. |
| Prolonged QT | Can be medication-related, electrolyte-related, inherited, or transient. | Review meds, electrolytes, and family history. Repeat ECG may be recommended. |
| Bundle branch block RBBB/LBBB |
Electrical delay in a heart “wire”. RBBB is often incidental; LBBB may be more significant. | Often prompts an echo to assess heart structure and pumping function. |
| ST-T changes “non-specific” or “ischaemic changes” |
Can be benign/non-specific, but in the right context can suggest reduced blood supply. | Symptoms decide urgency. Chest pain with ST changes needs urgent assessment. |
| Left ventricular hypertrophy | Thicker heart muscle; sometimes from high blood pressure, athletic training, or valve issues. | Echo is often used to confirm thickness and check valves. |
| Axis deviation | Can be normal; can also reflect body habitus, lung disease, or conduction patterns. | Usually interpreted alongside other findings rather than alone. |
If your report mentions “possible old infarct” or “septal infarct — age undetermined”, don’t panic. These phrases are commonly generated by ECG software and are a classic example of why correlation (symptoms + history + sometimes echo) matters.
This is the part most people actually need. The ECG is data — your symptoms tell us how urgent it is and which test is most useful next.
An ECG result can be reviewed later. If you feel seriously unwell right now, urgent assessment comes first.
If you’re trying to decide whether you need echo imaging, see: Symptoms that require an echo. If you want the basics first, start with: What is an ultrasound echo?
Different tests answer different questions. A short ECG is great for “what is happening right now”. Monitoring and ultrasound add context when symptoms are intermittent or when structure matters.

Useful if the first recording had artefact, symptoms have changed, or a clinician wants to compare patterns.

Captures rhythm over time — ideal for palpitations that come and go, dizziness episodes, or suspected ectopics.
If the ECG suggests hypertrophy, conduction problems, or you have breathlessness/swelling, echo can assess valves, chamber size, and heart function.
If you’re seeing terms like “LVH”, “bundle branch block”, “possible cardiomyopathy”, or you have symptoms like breathlessness, ankle swelling, or reduced exercise tolerance, an echo often becomes the “next best question” — because it tells you whether the heart’s structure and pumping match the ECG story.
Use the triage page: Symptoms that require an echo .
These are the questions patients usually ask right after reading their ECG report.